【出典】
World Health Organization, Department of Reproductive Health and Research: (2012). Safe abortion: technical and policy guidance for health systems. Second edition. WHO, 2003
【原文】
2.2.4 Surgical methods of abortion
2.2.4.1 Vacuum aspiration
The recommended surgical technique for abortion up to gestational age less than 15 weeks is vacuum aspiration (57). The high efficacy of vacuum aspiration has been well established in several randomized controlled trials. Complete abortion rates between 95% and 100% are reported (55, 56). Electric and manual vacuum technologies appear to be equally effective; however, the use of manual vacuum aspiration is associated with less pain in pregnancies under 9 weeks' gestation and with more procedural difficulty over 9 weeks' gestation (57). Vacuum aspiration under 14 weeks' gestation is more effective and associated with fewer minor complications than medical abortion (56, 58).
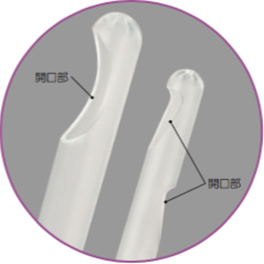
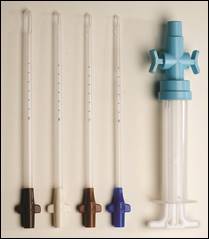
Vacuum aspiration involves evacuation of the con- tents of the uterus through a plastic or metal cannula, attached to a vacuum source. Electric vacuum aspiration (EVA) employs an electric vacuum pump. With manual vacuum aspiration (MVA), the vacuum is created using a hand-held, hand-activated, plastic 60 ml aspirator (also called a syringe). Available aspirators accommodate different sizes of plastic cannula, ranging from 4 mm to 16 mm in diameter. For each procedure, the appropriately sized cannula should be chosen based on the gestational age and the amount of cervical dilatation present; generally, the diameter of the cannula corresponds to the gestational age in weeks. Some cannula and most aspirators are reusable after being cleaned and high-level disinfected or sterilized. Foot-operated mechanical pumps are also available.
Depending on the duration of pregnancy, abortion with vacuum aspiration takes from 3 to 10 minutes to complete and can be performed on an outpatient basis, using analgesics and/or local anesthesia. The completion of abortion is verified by examination of the aspirated tissue. In very early pregnancy, the cannula may be inserted without prior dilatation of the cervix. Usually, however, dilatation using mechanical or osmotic dilators, or pharmacological agents such as misoprostol or mifepristone, is required before insertion of the cannula (see Section 2.2.1). Generally, vacuum-aspiration procedures can be safely completed without intrauterine use of curettes or other instruments. No data suggest that use of curettage after vacuum aspiration decreases the risk of retained products (59).
Most women who have a first-trimester abortion with local anesthesia feel well enough to leave the health-care facility after observation for about 30 minutes in a recovery room. Longer recovery periods are generally needed for abortions performed later in pregnancy and when sedation or general anesthesia has been used.
Vacuum aspiration is a very safe procedure. A study of 170 000 first-trimester abortions conducted in New York City by vacuum aspiration reported that less than 0.1% of the women experienced serious complications requiring hospitalization (60). Though rare, complications with vacuum aspiration can include pelvic infection, excessive bleeding, cervical injury, incomplete evacuation, uterine perforation, anesthetic complications and ongoing pregnancy (1, 2). Abdominal cramping and menstrual-like bleeding occur with any abortion procedure.
2.2.4.2 Dilatation and curettage
D&C involves dilating the cervix with mechanical dilators or pharmacological agents and using sharp metal curettes to scrape the walls of the uterus.
D&C is less safe than vacuum aspiration (61) and considerably more painful for women (62). Therefore, vacuum aspiration should replace D&C. The rates
of major complications of D&C are two to three times higher than those of vacuum aspiration (3). Randomized controlled trials comparing D&C with vacuum aspiration found that, for up to 10 weeks since the LMP, vacuum aspiration is quicker and associated with less blood loss than D&C (63, 64).
Where it is still practiced, all possible efforts should be made to replace D&C with vacuum aspiration, to improve the safety and quality of care for women. Where no abortion services are currently offered, vacuum aspiration should be introduced rather than D&C. At sites where vacuum aspiration has yet to be introduced, managers must ensure that proper pain- management protocols are followed, and that D&C procedures are performed by well-trained staff under adequate supervision.
【邦訳】
1.妊娠15週までの人工妊娠中絶に推奨される外科的中絶法は吸引法である。
2.吸引法には電動式と手動式(MVA)があり、どちらの方法も完全中絶率は95~100%で、有効性に差はみられない。
3.MVAでは妊娠9週未満で疼痛が相対的に少ないが、9週を越えると手技的に難しくなる。
4.妊娠14週未満の吸引法は、薬剤を用いる中絶よりも有効で合併症が軽く、少ない。
5.MVAでは、容量60mLのプラスチック製吸引器(シリンジともよばれる)で真空状態を作り出す。カニューレはプラスチック製で直径4~16mmのサイズがある。妊娠期間および子宮頸部拡張度に基づいて適切なサイズのカニューレを選択する。
6.吸引法による手術時間は妊娠期間に応じ3~10分である。鎮痛薬および/または局所麻酔を使用すれば外来での実施が可能である。
7.初期の妊娠では、子宮頸部を事前に拡張することがなくカニューレを挿入できる場合があるが、通常はカニューレの挿入前に拡張器、浸透性拡張剤、またはミソプロストールやmifepristoneなどの薬剤を利用した拡張が必要である。
8.一般的に、吸引法はキュレットやその他の器具を使用しなくとも安全に実施することができる。吸引後の追加の掻爬が受胎産物の残留リスクを減らすデータない。
9.局所麻酔(傍頸管ブロック)で行われた初期の吸引法による人工妊娠中絶は、回復室で30分程度の観察を行えば帰宅できるまでに回復する。一般に、妊娠期間が長いほど回復に時間がかかり、鎮静薬や全身麻酔を使用した場合も長い回復時間を要する。
10.吸引法による初期人工妊娠中絶17万例の調査では、入院を要する重篤な合併症の発現は0.1%に満たなかった。稀に吸引法の合併症として、骨盤内感染症、大量出血、子宮頸管損傷、内容遺残、子宮穿孔、麻酔に伴う合併症および妊娠継続が起こりうる。